Men and Women in Postnatal Family Health Services
Marg Bigsby, Harald Breiding-Buss, Evelyn Tritschler
Presented to the PHA Conference
Dunedin, 26 June 2002
Introduction
Involving fathers in services targeting the health and wellbeing of children and families has become an issue receiving increasing attention from the providers of such services. There are, however, a lack of models that could show how more and appropriate father involvement could be achieved.
Canterbury Plunket has been trying over the last two years to involve the partners of women suffering from postnatal distress to assist both the woman’s healing and her partner’s own adjustment process, by involving a worker from the Father&Child Trust.
This paper reports on the experiences from this co-operation, and how it could possibly be used as a model for other service providers who wish to involve men more in their services.
We report on the experiences of both men and women in the programme as they present them to their respective staff, also how their concerns are different and yet relate to the same problems and to the same family.
We will then outline how working with both partners in a family relationship raised the awareness of both partners in the collaboration. This led to some changes in the delivery of the service and had positive spin-offs beyond the actual programme.
Lastly we will discuss why we think co-operation like this is needed in other programmes, and how our experience could possibly be emulated by other services.
Background
Since late 1999, the Canterbury Plunket Postnatal Adjustment Programme (PPNAP) has been working with women with suspected postnatal depression and/or difficulty adjusting to the parenting role.
The programme is aimed at meeting the needs of women who don’t require the assistance of Psychiatric Emergency Services, or Maternal Mental Health Services, yet are still struggling with what is available to them.
The programme has been utilising Plunket staff as their main referrers and is intended to deliver the following key service components:
* Assessment of women who are referred, or who self-report postnatal distress.
* Use of an acceptable depression screening tool in partnership with the woman and her family where appropriate.
* Postpartum group education through a planned 8-session programme Working with other services to ensure that individual pregnant and postnatal women accessing PPNAP services have their needs met in the most appropriate way.
* Community Education including other health professionals and community groups to increase knowledge and awareness of postnatal distress and depression.
The programme includes a service based on Maori Health principles and delivered by Maori staff (Oranga Whakamomori), as well as a component for women living in rural areas of Canterbury.
Referral criteria include having a baby under a year of age, self-reporting current distress (with an Edinburgh Postnatal Depression Scale score of 10+ if available/appropriate), or a history of past episodes of PND (Postnatal Depression).
Since September 1999, the programme has received more than 450 referrals.
PPNAP is a support programme. When entering the programme the client is assessed and the client’s particular needs are discussed with her.
About a fifth of clients then enter an eight-week group programme, while others receive individual short-term support, usually at home, depending on the assessment outcome and resources already available to the client.
Any assessed need for professional counselling and/or medication is discussed with the client, but not provided by PPNAP itself.
Postnatal Depression is a recognised major mental health problem, with between 10 and 20% of mothers being affected (McGill et al, 1995). That postnatal depression can also occur in men is not universally accepted; however some studies put depression issues for men around or after the birth of their child at similar levels of frequency to that of women (Harvey & McGrath, 1989; Lovestone & Kumar, 1993).
The PPNAP team recognises childbirth as a major change in life circumstances for both women and men, which requires significant adjustment. For men, changes in the relationship with their partners and finding themselves in non-stereotypical roles are two of the most prominent factors in fathers with depression symptoms that come to our attention.
Fathers have had some input into the programme almost since its inception in 1999, when group facilitators asked the women about the best ways to share issues of postnatal distress with partners.
The women asked for a joint evening with the partners as part of the group experience, where discussion could be shared both among women and between their partners. This male-facilitated partner session became a regular part of the group programme, and 70% of partners of women participants attended.
[Footnote: Women completing the group option of care numbered 78 over a 27 month period (15 groups), and represented 18% of referred clients in that time.
Participants are required to arrange for care of their child/ren during sessions, which the programme is unable to provide.
They must also be able to separate from their child/ren for this time. These two requirements are a barrier to a number of prospective participants. Attending the group requires significant commitment by participants, but is rewarding.
Feedback from the majority of participants indicates that the group programme had a positive impact on their recovery, and satisfied or exceeded their expectations in terms of process and outcome.]
In May 2001 the Health Funding Authority made a small amount of additional funding available to offer follow-up support for the partners of the programme’s clients beyond the ‘partner evening’ for a year, however it did not renew this contribution.
Though not formally part of the PPNAP contract, the programme had also been extended to provide one-on-one support for men with symptoms of depression in the first year after the birth of their child.
Referrals for this service were usually made by the men’s partners, although there were an increasing number of direct or self-referrals of men, especially as a result of group participation.
This paper deals not so much with the mental health issue of postnatal depression and its effect on men and women, as with the client’s experiences as service recipients in a changed social environment, where strictly defined gender roles are changing.
A limited number of programmes target families as a whole, however the Father&Child Trust/Plunket co-operation in the Postnatal Adjustment Programme is a “mainstream” health service that attempted to look at the support needs of both parents in a gender-specific and holistic way.
While Plunket’s universal health service is family focussed and holistic in its approach, the interface tends to be with the mother for a variety of reasons common in parenting and health service providers (Breiding-Buss, 1999).
In some cases, this can lead to a bias in the interpretation of the health issues which can result in problems in a family environment, where stereotypical roles of “primary provider” and “primary caregiver” have changed.
Men’s perceptions as service recipients
Researchers in Nelson (Chapman, McIntosh &Mitchell, 2000) have found that health and social support services for families fail to reach fathers, and that this failure is associated with both, misconceptions of men as service recipients by the service provider as well as misconceptions by men of the service.
The same research team then studied the issue in association with Nelson Plunket for that organisation and found a lack of knowledge (but not commitment or willingness) about how to provide a service to fathers.
There are a number of structural barriers to male involvement across the whole range of education and health services targeted at families of young children (Breiding-Buss, 1999).
The issue has gained importance with an apparently increasing number of men spending significant time with primary responsibility for their young children, but having little access to parenting information and support services.
Working with the men in PPNAP gave staff an insight into the mechanisms and roles a service provider may play in determining the outcome of care. Some perceptions that the fathers brought up during group sessions, or during one-on-one sessions with their support worker, were:
* a lack of involvement and information about their partner’s treatment, even though the men may have been the ones who have encouraged the partner to seek help in the first place. A recently completed internal evaluation found that many men had commented that adding another group session with the men to the programme would be useful.
* being the subject of much verbal and emotional, sometimes physical abuse
In this context many men feel decidedly uncomfortable about their partners talking about this perceived lack of support by some men with other participants in their group or with Plunket staff.
Some of the men felt that they were blamed for their partner’s problems, perceived that their view was outnumbered by those of their partner and the worker, and that they were powerless to change the situation.
The unexpected difficulties for a family where a mother suffers postnatal distress or depression add to the father’s own adjustment to his role change.
Many fathers with partners affected by postnatal depression demonstrate symptoms or identify with symptoms of depression themselves. (Harvey &McGrath, 1988; Lovestone & Kumar, 1993; Ballard et al, 1994)
Where the men themselves are – or appear to be – affected by depression we encountered referral problems. Both identifying their own symptoms as those of depression and seeking help are difficult for men and women alike, because of the nature of the illness and the stigma attached to it.
Plunket nursing staff who are the programme’s referrers in two thirds of all cases, do not commonly see fathers during “well child” checks (Plunket’s main service contract) or additional contacts.
As a result, the staff would not often have the opportunity to observe symptoms of depression in new fathers, nor necessarily the experience to address them. A common referral for partner support would be initiated by the father’s partner, who had voiced her concerns for how her partner was coping.
Referral through the father’s partner brings its own problems.
New fathers typically feel vulnerable about their role in the family – the idea that their partner is talking about him to professionals with suggestions that he is not ‘pulling his weight’ can be very threatening to a struggling/depressed father.
He may not accept to be referred, for fear that he will not receive support, but instead advice and perhaps perceive criticism of how he performs his roles as father and husband. The Nelson research revealed that fathers perceive child and family-related services as services for their partners.
(If they are invited to participate, they attend as support people.) From this perception arises doubts for the intended recipients about the effectiveness of a service that targets fathers directly: they do not expect to be supported by the service, but to be trained to be supportive of others.
Contacting a father in situations where the partner has reported signs of difficulty adjusting to a new role, or depression poses ethical questions well known to health professionals working with men or women who have not yet accepted that they may suffer from a mental illness.
There is anecdotal evidence from separated clients of the Father&Child Trust that postnatal depression may be associated with relationship breakups.
Where postnatal depression has been diagnosed in the woman in relationships that have existed for 3-10 years, but broken up in the first 18 months after the baby’s birth, some men have attributed the relationship failure to the occurrence of postnatal depression.
However, Meighan et al (1999, p203) state “it is not known whether depression is the cause or the result of marital difficulties”.
Women’s perceptions as service recipients
Some of the experiences of women clients of PPNAP were consistent with the following themes.
In some cases, expectations of role changes prior to the baby’s birth had either not been explored to any significant degree by the parents, or were unrealistic. Sometimes, big decisions about roles were made on the basis of ‘choices’ over which the couple had little control (eg. economic, or employment-related).
* Some women identified that their partners were anxious for a rapid recovery from PND once a diagnosis was made and accepted. They reported that it was difficult for their partners to not be able to ‘fix’ it.
* Many women found it difficult dealing with the symptoms of PND, in particular when they had some awareness of their behaviour, but little control over it. This also included times when their mood was not congruent with anticipated occasions. For example, looking forward all day to their partner coming home in the evening, and being pleased and relieved when it occurred, but outwardly demonstrating irritability or frustration.
* Some women reached a point of considering using medication as part of their treatment, but said they were not supported in this decision by their partners.
*A small number of women said that their partners believed that their participation in the group programme was detrimental to their condition, and did not approve of the support these women sought and gained in utilising this option of care.
An internal evaluation recently completed of PPNAP looked at several aspects of the programme.
On reviewing the Edinburgh Postnatal Depression Scale scores of group participants, the vast majority of scores had decreased by an average of 8.9 points at the completion of the group, compared to at the time of referral, with the majority of these being under 12 points.
These indicate an improvement in women’s mood and greater wellness with respect to PND.
A principal benefit of the programme was when communication between partners had deteriorated, sharing information about the adjustment process to change, and specific education about depression and strategies to treat and manage it.
This gave many couples the ability to understand the situation they were in, and that it wasn’t a new ‘status quo’ for their relationship.
Working together
Working with only one parent in a service for difficulties around adjusting to role changes that affect the whole family inevitably means that the health worker is presented the issues from only one perspective.
When a health worker addresses the needs of their client, there is potential for a lack of understanding of the issues from the client’s partner’s perspective.
The partner may feel that the worker is working for their client alone, and not the family unit, if the partner’s experiences of the issues are not solicited and known. This could give rise to tension between the client’s partner and the client’s worker.
Professional services, such as Plunket’s Well Child Service, deliver care to the whole family from a holistic framework.
The staff consider the child client as the primary client, and view issues from the perspective of each family member, in addition to seeing the family within the socio-cultural context it lies in. This model of family nursing is also the basis for care by staff of PPNAP.
However, when the opportunity arose for PPNAP to engage the services of a male health worker, the ability of the programme to assess and address the issues of both adult partners in the family in a gender specific way was significantly enhanced.
Cultural constructs of male and female mean that men and women have different ways of doing the same things, different ways of communicating and different social ways.
The hesitancy of the male clients of PPNAP to access the service initially, reflects male perceptions about such services in general, and presents a major barrier to service delivery.
However the PPNAP experience also shows that such difficulties can be overcome in a mixed gender team that respects different approaches.
Breiding-Buss (2000a) developed a model showing how a combination of factors exert influences on the different relationships within the family, and on either parent’s commitment to paid work. These influences can be categorised as either coming from institutions (including health or parent service providers), or from society, in the form of particular stereotypes and images.
The involvement of a male worker at the interface between service and recipient/s by a Plunket programme has not only supplemented the service, but has encouraged new thinking about the aims and delivery of PPNAP care.
As a result, some changes were made to the original programme.
This collaboration has had spin-offs for other Plunket services as well, including a change in awareness of fathers’ issues as perceived by Canterbury Plunket’s team.
This may well influence and improve the acceptability of the service to fathers and permit their greater involvement in delivering Well Child Health services to their children.
Through the co-operation with the Father&Child Trust, Plunket was also able to gain better access to resources made by and targeted at fathers, which helped to reach fathers better. The Trust, in turn, benefited from Plunket’s professional know-how and gained much better insight into policy and practice of professional health and social services.
This assisted the Trust’s evolution from a community organisation to a service provider, and the association added much credibility to the Trust’s work.
The key ingredients to the successful co-operation are:
* an ongoing awareness by the Plunket team that including fathers in care will improve outcomes for mothers and babies.
* empathy for a father’s own mental state, and an awareness that untreated or prolonged distress impacts negatively on the baby’s development.
* openness to new ideas and approaches having the male worker supported by an organisation with practical expertise in working with fathers and its own support mechanisms and resources good communication between staff working with the same family an appreciation of what either programme partner can learn from the other.
One person may struggle more with postnatal adjustment issues than their partner, and the less affected person may exhibit symptoms of such distress largely as a result of the difficulties arising from their partner’s illness.
Under current service specifications, even when the father is the more distressed partner, the mother may be the one who qualifies for, and receives, support from a postnatal health service. While the male health worker was employed, PPNAP had greater opportunity to assess and address fathers adjustment needs after the birth of a baby.
In some instances both partners receiving support from PPNAP staff reported emotional and verbal abuse by the other to their respective female and male workers, and both workers were under the impression that this abuse was one-sided.
Debriefing by the workers working with the individuals revealed a more comprehensive picture of the relationship that both would have been otherwise unaware of. Morgan, et al (1997, p914) state that it is important to “treat the couple”.
A Model for Other Services?
A study by the Office of the Children’s Commissioner (Julian, 2000) has found overwhelming support amongst the New Zealand public for a shared approach to parenting.
92% of the 2000 survey respondents agreed with the statement that “fathers should be expected to take an equal role in parenting”. The idea that looking after young children is “not manly” was also rejected by 94%.
Programmes such as Plunket’s “Tot’s & Toddlers” are targeting single -sex boys schools, among others, with parent craft courses. This helps to develop expectations in young men to be accepted and respected as parents.
But meeting such expectations will have to include better access for men to services and institutions targeting parents and children.
It is a premise of this Model by Breiding-Buss that the current service systems for care of children and their families unintentionally encourage a role-split model which is not now supported by the New Zealand public overall.
This occurs by the services being largely available during ‘working’ hours during weekdays when men are often at their place of employment, staff who teach and model child health care expertise are predominantly female, and historically by the organisations primarily working to meet the needs of mothers and babies.
In a contemporary social environment with different social expectations, and during a time of many changes and adjustments in a couple’s relationship due to the birth of a new baby, these systems may in some cases have become a contributor to some of the problems they seek to address.
It is especially important to pre-empt the perception by fathers that they are not considered worthy service recipients in their own right.
The co-operation between the Father&Child Trust and Canterbury Plunket is a model that can be emulated by other services.
With the Father&Child Trust, Canterbury Plunket has had access to a small but reasonably well established organisation that has accumulated practical expertise in working with male parents. While fathers’ groups exist in other parts of New Zealand, most of these are focussed on advocacy and lobbying especially on behalf of separated fathers rather than service provision.
In addition there is an extreme shortage of qualified male family health workers and parent educators. Most organisations will, however, have access to a pool of men that could be used to supply some male ‘faces’ to organisations where women are the staff interfacing with clients.
Consistent male input into such services is likely to change its delivery, and an openness by the organisation to allow that to happen is the most important ingredient in a successful co-operation.
The Plunket/Father&Child Trust co-operation has also shown that a certain structural independence of the group of fathers from the organisation delivering the service is important: otherwise a male worker could simply be absorbed into the structure or the organisation, without the changes occurring that will secure continuous involvement and input by men.
Service Provider Involvement With Families
Model adapted from Breiding-Buss (1999)
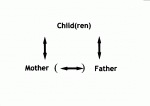 (1) Both parents desire a meaningful and significant relationship with their children. Mother and father may or may not be in a relationship with each other.
(1) Both parents desire a meaningful and significant relationship with their children. Mother and father may or may not be in a relationship with each other.
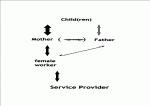 (2) Intervention of a service provider, often targeted at – or for the benefit of – the child, occurs through female workers establishing a relationship with the mother of the child.
(2) Intervention of a service provider, often targeted at – or for the benefit of – the child, occurs through female workers establishing a relationship with the mother of the child.
The mother-child relationship is strengthened through the intervention – but possibly at the expense of other relationships within the mother-father-child triangle.
Individual workers sometimes work with the father also, but effectiveness may be limited.
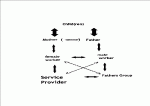 (3) Effects of involving a fathers group in the service. The lack of male workers in the professions can be bridged through the involvement of a fathers group. Service provider and fathers group influence each other’s policies and practice.
(3) Effects of involving a fathers group in the service. The lack of male workers in the professions can be bridged through the involvement of a fathers group. Service provider and fathers group influence each other’s policies and practice.
Parents receive individual support that strengthens the mother-father-child triangle as a whole. Feedback from practice into policy now involves experiences from working with men as well.
References:
Ballard, C., Davis, R, Cullen, P., Mohan, R., Dean, C. (1994); “Postnatal depression in mothers and fathers”, British Journal of Psychiatry, Vol 164, pp782-788.
Breiding-Buss, H. (1999) “Developing Support Services For Fathers” in: Birks S, Callister P: ‘Perspectives on Fathering II’, Centre for Public Policy Evaluation, Massey University.
Breiding-Buss, H. (2000a) “Supporting a Team Approach in Parenting: A New Vision For Parent Support in: Issues Paper #10, Centre for Public Policy Evaluation, Massey University; pp 42-49.
/papers/supporting-a-team-approach-in-parenting-a-new-vision-for-parent-support/
Breiding-Buss, H. (2000b) “Involving Men in Maternity Services” in: Birks S (ed.) ‘Inclusion or Exclusion: Family Strategy and Policy’, Issues Paper #9, Centre for Public Policy Evaluation, Massey University; pp 1-8
Chapman P., McIntosh, C, Mitchell, D (2000): “Real Dads-Real Men: A Study of Father’s Experiences of Child and Family Services”. in: Birks S (ed.) ‘Inclusion or Exclusion: Family Strategy and Policy’, Issues Paper #9, Centre for Public Policy Evaluation, Massey University, pp 9-26.
Harvey, L., McGrath, G. (1988); “Psychiatric morbidity in spouses of women admitted to mother and baby units”, British Journal of Psychiatry, Vol 152, pp506-510.
Julian R.:”Fathering in the New Millenium” (2000); Office of the Children’s Commissioner, Wellington.
Lovestone, S., Kumar, R.(1993); “Postnatal psychiatric illness: impact on partners”, British Journal of Psychiatry, Vol 163, pp210-216.
McGill, H., Burrows, V., Holland, L., Langer, H., Sweet, M. (1995); “Postnatal depression: a Christchurch study”, New Zealand Medical Journal, pp162-164, 10 May.
Meighan, M., Davis, M., Thomas, S., Droppelman, P. (1999); “Living with Postpartum Depression: The Father’s Experience”, MCN, Vol 24, No 4, pp202-208, July/August.
Morgan, M., Matthey, S., Barnett, B., Richardson, C. (1997); “A group programme for postnatally distressed women and their partners”, Journal of Advanced Nursing, Vol 26 , 913-920.




